In my 25 years in the insurance business I’ve seen many changes. But there’s always been one constant: Healthcare and pharmacy costs continue to accelerate and no regulatory action has been able to slow this runaway train. The problem is that we have focused on the wrong end of the spectrum. We don’t have a healthcare issue; we have a billing issue.
At the root of this national crisis is a lack of
But that could change with
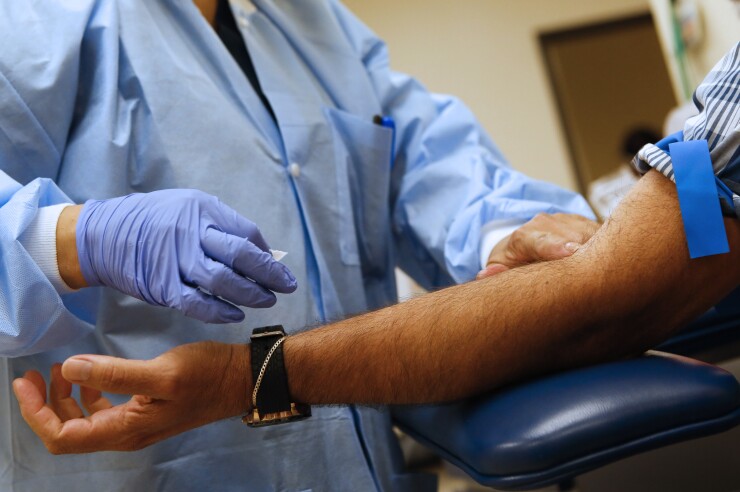
Here’s how it works.
Reference-based pricing attacks the problem from all angles and targets billing — which is at the heart of the crisis.
Typically, a preferred provider organization network achieves a 50-60% discount on billable charges. However, after this 50-60% discount, the cost of care is still double or triple what Medicare pays for the same service. For example, the same cholesterol blood test can range from $10 to $400 at the same lab. The same hospitalization for chest pain can range anywhere from $3,000 to $25,000.
Reference-based pricing allows employers to pay for medical services based on a percentage of CMS reimbursements (i.e. Medicare + 30%), rather than a percentage discount of billable charges. This model ensures that the above-mentioned hospitalization cost an employer $3,000 rather than $25,000.
“Negotiating” like Medicare
Reference-based pricing is becoming increasingly popular as more organizations consider the move to correct cost transparency issues as they transition from fully-insured to self-funded insurance plans.
One well-known and considerable example is Montana’s state employee health plan. The state employee health plan administrator received a notice from legislators in 2014 urging the state to gain control of healthcare costs. Instead of beginning with hospitals’ prices and negotiating down, they turned to reference-based pricing based on Medicare. Instead of negotiating with hospitals, Medicare sets prices for every procedure, which has allowed it to
The state of Montana set a reference price that was a generous 243% of Medicare — which allowed hospitals to provide high-quality healthcare and profit, while providing price transparency and consistency across hospitals. So far, hospitals have agreed to pay the reference price.
See also:
Of course, there is still the risk that a healthcare provider working with the state of Montana health plan, or any other health plan using reference-based pricing, could “balance bill” the member. But a fair payment and plenty of employee education about what to do if that happens could help you curb costs.
If balance billing does occur, many solutions include a law and auditing firm to resolve the dispute. In one recent example, a patient was balance billed almost $230,000 for a back procedure after her health plan had paid just under $75,000. An auditing firm found that the total charges should have been around $70,000, and a jury agreed. The hospital was awarded an additional $766.
Reference-based pricing is a forward-thinking way to manage costs while providing high-quality benefits to your employees. It’s one way to improve cost transparency, which may eventually transform the way that we buy healthcare.





